Introduction
Adequate nutrition during infancy and early childhood is essential to ensure the growth, health and development of children to their full potential.1 It has been recognised worldwide that breastfeeding is beneficial for both the mother and child, as breast milk is considered the best source of nutrition for an infant.2 Economic and social benefits are also provided to the family, the health care system and the employer.
The World Health Organization (WHO) recommends that infants be exclusively breastfed for the first six months, followed by breastfeeding along with complementary foods for up to two years of age or beyond.3 Exclusive breastfeeding can be defined as a practice whereby the infants receive only breast milk without mixing it with water, other liquids, tea, herbal preparations or food in the first six months of life, with the exception of vitamins, mineral supplements or medicines.4 Breastfeeding an infant exclusively for the first 6 months of life carries numerous benefits such as lowered risk of gastrointestinal infection, pneumonia, otitis media and urinary tract infection in the infant while mothers return to her pre-pregnancy weight very rapidly and have a reduced risk of developing Type 2 diabetes.5,6, 7
Moreover, studies have shown that many mothers find it difficult to meet personal goals and to adhere to the expert recommendations for continued and exclusive breastfeeding despite increased rate of initiation.8 Some of the major factors that affect exclusivity and duration of breastfeeding include breast problems such as sore nipples or mother’s perceptions of producing inadequate milk4,9,11 and societal barriers such as employment, length of maternity leave,9 inadequate breastfeeding knowledge,11 lack of familial and societal support and lack of guidance and encouragement from health care professionals.2,9
Another factor that leads to early cessation of breastfeeding is the advertisement of infant formulas which encourages mothers to opt for the use of pacifiers and bottle feeding.3,9 Additionally, many mothers opt for breast milk substitutes because they need to resume work while others claim that they produce insufficient milk.10 To date, there are various types of infant formulas available on the market, and which are designed to meet the nutritional needs of infants with a variety of dietary needs.12 However, there are some problems associated with infant formulas such as the nutritional content either does not meet or exceeds the infant’s needs. For instance, it was reported that some infants who were fed on formula milk have had occasional water soluble vitamins deficiencies.13 Another problem associated with bottle feeding involves high risk of exposing the child to pathogens owing to unhygienic practices during handling and preparation of infant formula.3
On the other hand, when breast milk or infant formula no longer supplies infants with required energy and nutrients to sustain normal growth and optimal health and development, solid foods should be introduced.14 This process is known as complementary feeding. According to the WHO recommendations, the appropriate age at which solids should be introduced is around 6 months 15 owing to the immaturity of the gastrointestinal tract and the renal system as well as on the neuro-physiological status of the infant.15 However there are concerns about the timing of complementary feeding as evidence demonstrates that this recommendation for delayed introduction of complementary foods may have detrimental consequences.17 Furthermore there are different types of weaning that mothers adopt namely child-led/natural, mother-led, gradual, partial or abrupt weaning.18 It should be noted that during the weaning process many mothers encounter infant feeding problems such as refusal-to-eat, colic, and vomiting among others.19 All these problems that mothers encounter during the feeding processes either directly or indirectly influence the feeding pattern.
The objectives of this study are to:
- Appraise the advantages of exclusive breastfeeding.
- Provide an overview of problems which hinder the practice of breastfeeding among mothers.
- Discuss the appropriateness of complementary feeding and feeding difficulties which infants encounter.
Breastfeeding Practices
The determinants of children’s growth include genetic potentialities, family size, lifestyle, socio-economic environment, infections, nutrition and the availability of medical care.20 However, nutrition is the most prominent factor which can either directly or indirectly influences children’s future development. For instance, those children who are malnourished and manage to survive do not enjoy a good health and experience impaired development in the long run.21 Along, there is a rising concern about overweight and obesity in children. Therefore, proper nutrition and nurturing during the early years of life is crucial for an infant to achieve optimal health and well-being. Hence, there is no more precious gift in infancy than breast feeding.
“Breastfeeding is an unequalled way of providing ideal food for the healthy growth and development of infants; it is also an integral part of the reproductive process with important implications for the health of mother”.22
Saha et al.,23 reported that the current recommendations of WHO and UNICEF on breastfeeding are as follows
- Initiation of breastfeeding within the first hour after the birth.
- Exclusive breastfeeding for the first six months.
- Continued breastfeeding for two years or more and proper introduction of solid foods starting in the sixth month which are nutritionally safe and adequate.
Exclusive Breastfeeding
Exclusive breastfeeding as defined by WHO and UNICEF is the practice whereby an infant receives only breast milk from the mother or a wet nurse or expressed breast milk.24 The WHO and UNICEF, both recommend that mothers should breastfeed their child exclusively for the first 6 months and continue breastfeeding up to 2 years or longer rather than stop EBF practice as from 4-6 months.25
Although breastfeeding an infant exclusively for the first 6 months of life carries numerous benefits, many studies are centered on the “weanling’s dilemma” in developing countries which involves choosing between the protective effects of exclusive breastfeeding against infectious diseases and the (theoretical) insufficient breast milk to meet the infants’ energy and micronutrient needs beyond four months of age.26 However, the author claimed that there is no data giving an estimate of the proportion of exclusively breastfed infants at risk of specific nutritional deficiencies.
Expressed Breast Milk
Breastfeeding is beneficial both to the infant and the mother.27 However, owing to certain circumstances, mothers are unable to breastfeed, so they wish to express their milk because it is the only opportunity for the infant to have the human milk.28 Expressing is simply a way of taking milk from the breast without the baby suckling and this can be achieved either by the hand or manual pump or electric pump.29 The reasons why some mothers express breast milk are shown in Figure 2.1.
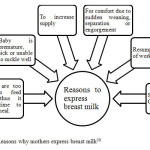 |
Figure 2.1: Reasons why mothers express breast milk30 |
While breast milk in a bottle is far superior to any infant formula, expressing or pumping breast milk do have some disadvantages unlike direct breastfeeding as shown in Figure 2.2.
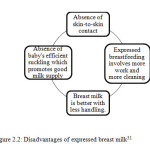 |
Figure 2.2: Disadvantages of expressed breast milk31 Click here to View Figure |
Composition of Breast Milk
Human milk is species-specific and is superior to any other breast milk substitute32 and it is also assumed to the ideal food for infant during the first 4-6 months, ensuring proper growth and development.33 Human milk which is the most natural food available for infant is unique whereby its nutritional composition varies from mother to mother, from day to day, during the day and during a feed.34, 35 Human milk contains several factors such as immunoglobulin, T lymphocytes, enzymes such as lysozymes, phagocytes among others which are not present in breast milk substitute.36 A comparison of composition of human colostrum, human mature milk, cow’s milk and standard formula is depicted in Table 2.1.
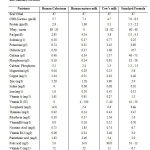 |
Table 2.1: Comparison of composition of human colostrum, human mature milk, cow’s milk and standard formula37 |
Characteristics of Breast Milk
“Breast milk is unique in its physical structure and types and concentrations of protein, fat, carbohydrate, vitamins and minerals, enzymes, hormones, growth factors, host resistance factors, inducers and modulators of the immune system, and anti-inflammatory agents”.12 There are three phases of milk namely, colostrum, transitional milk and mature milk each with distinct characteristics.
Infant’s first milk
The first milk that is synthesized by the breast for the baby right after birth is thick, yellow-coloured fluid called colostrum. The yellow color is owing to the high concentration of beta-carotene, a precursor of vitamin A which is required for the protection against infection and for early retinal development.38 It has also been stated that the amount of colostrum obtained is limited but it rich in nutrients and substances that the infant needs in the first days of life.12 The “liquid gold” is rich in proteins, fat-soluble vitamins, minerals, and immunoglobulins A- sIgA.33 It should be noted that IgA protects the infant’s immune system by identifying and destroying foreign objects such as bacteria and viruses.12 Another advantage of colostrum is that the mother will have less blood loss because the uterine contracts as the baby suckle. Furthermore, colostrum also contains white cells which help to prevent infection in the infant and it also consists of lactose which prevents hypoglycemia and at the same time helps the newborn to pass meconium.38 This in turn, promotes the excretion of bilirubin.
Transitional milk
Transitional milk is used to describe the postcolostral period (7 to 21 days post partum) when the composition of the milk changes more slowly than in the first few days following parturition.39 The content of transitional milk includes high levels of fat, lactose, water-soluble vitamins, and contains more calories than colostrum but lower levels of immunoglobulins.33
Mature milk
Mature milk (21 days post partum) also varies but to a lesser extent than in early lactation.39 Mature milk looks thinner, paler and is more watery than colostrum.33 Additionally, it consists of 90% water which is required to maintain hydration of the infant and the remaining 10% consists of carbohydrates, proteins and fats which are important for both growth and to meet energy needs of the baby. There are two types of mature milk: Foremilk and hind- milk.
Foremilk
Foremilk is the first milk available in large amount at the beginning of a feeding which is watery thus, providing all the water the baby needs from it. Therefore, no other drinks such as water or juice are required before 4-6 months, even in hot climate.40 Foremilk is rich in proteins, lactose and other essential nutrients but contains less fat.33
Hind-milk
Hind- milk is the richer milk, containing more fat which occurs after the initial release of milk and is more opaque and creamy white in colour.40 This type of milk induces a feeling of satiety in the infant as well as making the latter feels sleepy.12
Therefore, both foremilk and hind-milk are necessary for the baby to receive optimum nutrition in order to grow and develop well.
Advantages of Breastfeeding
Breastfeeding is universally endorsed by the world’s health and scientific organizations as the best way of feeding infants.41 Many studies have been carried out and have highlighted innumerable benefits of breastfeeding for infants, for mothers and the society. Some of them include lowered risk of otitis media, gastroenteritis, respiratory illness, sudden infant death syndrome, necrotising enterocolitis, obesity, hypertension among others in infants42 (Table 2.2). Maternal outcomes include reduced risk of breast and ovarian cancer, Type 2 diabetes, and postpartum depression (Table 2.3) while societal benefits include decrease health care related cost and fewer absences from work.
 |
Table 2.2: Benefits of breastfeeding 46 |
 |
Table 2.3: Benefits of breastfeeding for mothers37 |
Concerns, Controversies And Contraindications To Breastfeeding
Although breastfeeding is optimal for infants, there are some controversies surrounding breastfeeding and very few contraindications. Breastfeeding is contraindicated due to the following
- In infants who have special health problems such as galactosemia, maple syrup urine disease and phenylketonuria.38
- In cases where mothers have active untreated tuberculosis disease or are human T-cell lymphotropic virus type I– or II–positive.32 Breastfeeding may not be in the best interest of the baby when breastfeeding mothers have herpes simplex lesions on a breast (infant may feed from other breast if it is free from any lesions).32
- In situations where the mother is using drugs of abuse.55
- In certain circumstances where mothers are receiving diagnostic or therapeutic radioactive isotopes,antimetabolites or chemotherapeutic agents, small number of other medications or who had been exposed to radioactive materials.32 They should not breastfeed until these substances are cleared from the breast milk.54
- In infants born to mothers who are HIV infected, breastfeeding is discouraged owing to the risk of transmission of HIV to the infant through human milk.54 Naylor &Wester38 highlighted thatWHO recommends replacement feeding if it is acceptable, feasible, affordable, sustainable and safe (AFASS).
Additionally, more and more studies are supporting the fact that if an HIV infected mother choose to or must breastfeed, it is essential to breastfeed exclusively for the first six months to reduce the risk of contaminants that may come with formula and other foods and cause gut inflammation allowing HIV organisms to reach the submucosal tissue.38 Furthermore, antiretroviral drugs can reduce the risk of HIV infection to the infant through breast milk.
Problems with Breastfeeding
Among mammals, the only species in which breastfeeding and weaning have to be learned and are not governed by instinct are the Homo sapiens56 and breastfeeding problems are very common, but last for a short time and are preventable.38 According to Giugliani,56 many mothers are facing breastfeeding problems as their traditional source of learning was lost as extended families are being replaced by nuclear families. This provides few opportunities for the mothers to learn about breastfeeding. Therefore, to enable a mother to start or continue enjoying the lactation process, prevention and treatment is recommended.
Breast engorgement
Breast engorgement is mainly caused by infrequent or ineffective milk removal.38 The breasts become engorged 3-5 days postpartum.57 The breasts become full, warm and at the time when the “milk comes in” at 3-5 days after delivery, there is a rapid increase in milk volume that cause vascular congestion which is followed by oedema.38 Excessive engorgement with pain and oedema can be avoided by adopting the practices as shown in Figure 2.3.
 |
Figure 2.3: Avoiding breast engorgement 54 Click here to View Figure |
Sore nipples/ nipple trauma
One of the reasons why mothers discontinue breastfeeding and opt for early weaning is owing to sore nipples.54 This usually occurs while the baby is latching during the first week or two and it eventually makes the women feel a mild pain and discomfort. According to Giugliani,56 the causes of pain during breastfeeding are shown in Figure 2.4.
 |
Figure 2.4: Causes of sore nipple 56 |
Sore nipples can be prevented by teaching proper techniques on the initiation of breastfeeding.58 Additionally, the breast should be allowed to air-dry for some minutes after a feeding and nursing pads should be changed regularly to prevent milk flow.56,57 Other precautions include expressing breast milk if the breasts are engorged and avoiding use of soap, alcohol and extra water on the breast.57
Insufficiency of milk
Another reason causing early termination of breastfeeding is insufficient breast milk.59 Most women produce sufficient milk according to the baby’s needs, however, the complaint of “insufficient milk” is not just owing to the wrong perception of the mother but the latter lacks confidence on her ability to breastfeed.56 Other reasons that make mothers perceive that they are not producing “sufficient milk” are ineffective suckling and/or infrequent feeding routines, conditions of the baby, such as illness or ankyloglossia, condition of the mother such as fatigue, stress, and use of certain medications, psychological inhibition, pregnancy, and smoking.38
Therefore, it is important to determine the aetiology of the milk insufficiency in order to identify necessary interventions to resolve the problem.60
There are many other problems that many mothers experience during the lactation process which include gigantomastia, plugged ducts, flat/inverted nipples, medical complications such as mastitis, breast abscess among others.54
Formula Feeding Practices
According to the National Academy of Sciences,61 multiple health organisations endorse breastfeeding as the optimal form of nutrition for infants for the first year of life. However, not all mothers are able to breastfeed either temporarily or permanently, owing to a small number of health conditions of the infant or the mother.62 Hence, many infants who were unable to be breastfed were wet-nursed (given breast milk by a woman other than the child’s mother) while others, who were unfortunate were “dry-nursed”. Dry nursing refers to home prepared mixture which consisted of a liquid, either water or milk mixed with finely ground grains. Over time, cow’s milk was modified to feed infants who were unable to breastfeed. Infant formulas are food products designed to provide for the nutritional needs of infants under 1 year old.63 They include powders, concentrated liquids, or ready-to-use forms. The first commercial infant formula consisted of wheat flour, cows’ milk, malt flour and potassium bicarbonate. Thereafter, new kinds of formula milk were developed whereby certain modifications were needed to make it safe and palatable for human infants.61 The birth of infant formula industry became more apparent owing to the process of modifying cow milk for large-scale production in the 1920s.
Currently, there are more than 40 formulas for healthy term infants which are being sold64 and FDA monitors infant formula manufacturers to ensure that the product provides the appropriate nutrition for all infants. Fisher64 pointed out that each product has a unique and desirable feature for optimal development of the infant as explained in Table 2.4.
 |
Table 2.4: Types of Infant formula12 |
Problems with Infant Formula
Formula feeding have some benefits such as convenience, fewer feeding times and mothers need not worry about their food or liquid intake being passed to the baby.65 However, infant formulas do have drawbacks as shown in Figure 2.5.
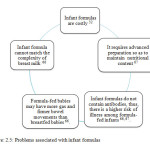 |
Figure 2.5: Problems associated with infant formulas |
Complementary Feeding
Complementary feeding is the term used for giving other foods and drinks in addition to breastfeeding after the completion of the 6 months exclusive breastfeeding period.69 According to WHO,7 this process covers the period from 6-24 months of age and is a critical period of growth during which infants are at high risk of nutrient deficiencies and illnesses.
The importance of introducing solid foods in addition to the infant’s milk feed is shown in Figure 2.6.
 |
Figure 2.6: Reasons for introducing solid foods 14 |
The ideal age to begin weaning is 4 to 6 months of age because besides filling the gap between the total nutritional needs of a child and the amounts provided by breast milk, it is the age when nerves and muscles in the mouth develop sufficiently to let the baby munch, bite and chew.68 Nevertheless, following the WHO recommendations in 2001 there has been considerable debate over the ideal age to begin weaning in healthy term infants.26 It has been highlighted that gastroenteritis is common in developing countries and is associated with the introduction of formula and complementary foods.14 It is to be noted that the risks of gastroenteritis is lower in developed countries, thus many are questioning whether the WHO recommendation applies for the developed countries as well.69 Furthermore, it was highlighted14 that the debate remains over whether some infants who are not weaned until 6 months may be at risk of micronutrient deficiencies.
Early and Late Introduction Of Complementary Foods
Timing of the first introduction of solid food during infancy may have potential effects on life-long health.70 It can be seen that very often solid foods are either given too early or too late. According to UNICEF,71 the frequency and amounts of food that is given may be insufficient hence;hindering the normal growth of the child or their consistency or energy density may be incorrect in relation to the child’s needs. Therefore WHO 72 stated that it is advisable for mothers to adopt an appropriate complementary feeding as shown in Figure 2.7:
Early weaning
Some studies have shown that giving solid foods too early may lead to increased risk of chronic diseases such as islet autoimmunity (the pre-clinical condition leading to Type 1 diabetes), obesity, adult-onset celiac disease, and eczema.70
Nevertheless, it was affirmed there is no evidence of harm even within populations that begin weaning within a few days of birth.14
 |
Figure 2.7: Appropriate complementary feeding72 |
Late Weaning
A study by Kuo et al.,70 has shown that late weaning may cause deficiencies of zinc, protein, iron and vitamins B and D that leads to the suppression of growth and cause feeding problems. Iron deficiency anaemia and rickets are also found to be more prevalent among infants who are weaned after 6 months.14
Types of Weaning
There are different ways by which weaning can happen. Table 2.5 shows the different types of weaning.
 |
Table 2.5: Types of weaning |
Complementary Foods
The best way to help a baby’s digestive system to get used to solid foods is by introducing the foods gradually and one new food at a time so that if the infant has had any allergy, it can be spotted easily.69 Starting new foods is a critical step for the baby and it usually takes some time for infants to get used to this new way of eating. It is usually best to start weaning (around 6 months) the infant with the foods shown in Figure 2.8.
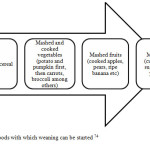 |
Figure 2.8: Foods with which weaning can be started 74 |
Common Feeding Difficulties in Infants
Many parents have concerns and questions about infant feeding and eating issues whereby the most common feeding difficulties are colic, poor appetite, food refusal or selective eating.75 It is important to treat feeding difficulties which can later leads to failure to thrive, nutritional deficiencies, impaired parent/child interactions and chronic aversion with socially stigmatizing mealtime behavior.76 According to Liu & Stein,77 feeding problems can be a result of medical disorders and inappropriate food selection. Some common feeding problems are depicted in Table 2.6.
 |
Table 2.6: Infant feeding problems |
Conclusion
Breastfeeding is the gold standard of infant feeding up to 6 months.It remains the most cost effective way for reducing the risk of diseases such as obesity, hypertension, eczema, type diabetes among others in later life as well as mortality. Breast engorgement, sore nipples, milk insufficiency and availability of various infant formulas are the main factors which influence breastfeeding practice in terms of initiation, exclusivity and duration. On the other hand, complementary foods in terms of nutrient-dense are normally introduced around 4 to 6 months. Difficulties encountered during the weaning process are often refusal to eat followed by vomiting, colic, allergic reactions and diarrhoea. Given related problems associated with breastfeeding, it is highly likely that in the future, nutrigenomics (or nutrigenetics) based research will provide opportunities towards personalized modification of breast milk for optimum health of neonates.78
References
- World Health Organisation, 2009. Infant and young child feeding. France: WHO.
- Ku C.M. and Chow S.K.Y., J. Clin. Nurs., 19, 2434 (2010).
CrossRef - Hanif H.M., Int. Breastfeed J., 6, 15, 1 (2011).
- Nkala T.E. and Msuya S.E., Int. Breastfeed J., 6, 17, 1 (2011).
- Kramer M.S. and Kakuma R., Cochrane Database Syst. Rev., 1, 1 (2009).
- Bai Y.K., Middlestadt S.E., Peng C.Y. J. and FLY, A.D., J. Hum. Nutr. Diet., 22 (2009).
- World Health Organisation, 2011. Promoting proper feeding for infants and young children [online]. Available from: http://www.who.int/nutrition/topics/infantfeeding/en/index.html
- Whalen B. and CRAMTON, R., Curr. Opin. Pediatr., 22, 5, 655 (2010).
- Thurman S.E. and ALLEN P.J., Pediatr. Nurs., 34, 5, 419 (2008).
- Sloan S., Sneddon H., Stewart M. and Iwaniec D., Child care Pract., 12, 3, 283 (2006).
- Cherop C.E., Keverange-Ettyang A.G. and Mbagaya G.M., East Afr. J Public Health, 6, 69 (2009).
CrossRef - United States Department of Agriculture, Infant Nutrition and Feeding, 3, 51 (2011).
- Miller S.A. and Chopra J.G., Am. Acad. Pediatr., 639 (2001).
- More J., Jenkins C., King C. and Shaw V., Brit. Diet. Assoc., 1 (2010).
- Brown A. and Lee M., Matern. Child Nutr., 7, 34 (2010).
CrossRef - Dratva J., Merten S. and Ackermann-Liebrich U., ActaPaediatr., 95, 818 (2006).
CrossRef - Prescott S.L., Smith P., Tang M., Palmer D.J., Sinn J., Huntley S.J., Cormack B., Heine R.G., Gibson R.A. and Makrides M., Pediatr. Allergy Immunol., 19, 375 (2008).
CrossRef - Bonyata, K., Flora, B. and Yount P., 2007. Weaning: How does it happen? [online]Breastfeeding and parenting. Available from: http://www.kellymom.com/bf/weaning/how_weaning_happens.html
- Hagekull B., Bohlin G. and Rydell AM., Inf. Mental Hlth. J.,18, 1, 92 (1997).
- Belkeziz N., Amor H., Lamdaour, Bouazzaoui N. and Baali A., Sociedad Española de AntropologíaBiológica, 21, 71 (2000).
- World Health Organisation, 2011. Complementary feeding [online]. Available from: http://www.who.int/elena/titles/complementary_feeding/en/
- Vehid H.E., Haciu D., Vehid S., Gokcay G. and Bulut A., Nobel Medicus, 5, 3, 53 (2009).
- Saha K.K., Frongillo E.A., Alam D.S., Arifeen S.E., Persson L.A. and Rasmussen K.M., Am. J. Clin. Nutr., 87, 1852 (2008).
- Labbok M., La Leche League Int., 19, 3, 19 (2000).
- Abba A.M., De Koninck M. and Hamelin A.M., Int. Breastfeed J.,5, 8, 1 (2010).
- Fewtrell M.S., Morgan J.B., Duggan C., Gunnlaugsson G., Hibberd P.L., Lucas A. and Kleinman R.E., Am. J. Clin. Nutr., 85, 635 (2007).
- Sadoh A.E., Sadoh W.E. and Oniyelu P., Nigerian Med. J., 52, 1, 7 (2011).
- Jones E., Dimmock P.W. and Spencer S.A., Arch. Dis. Child. Fetal Neonatal, 85, 91, 2011.
CrossRef - Babycentre, 2010. Expressing Breast milk [online]. Availablefrom:http://www.babycentre.co.uk/baby/breastfeeding/pumpingexpressing/expressingbreastmilk/
- South Eastern Sydney Illawarra Health, 2009. Expressing and storing breastmilk. Area Lactation Group: SESIH.
- Malabanan S.B., 2009. Pumping and expressing [online]. Available from: http://www.babycenter.com.ph/baby/breastfeeding/pumpingexpressing/exclusive-pumping-expert/
- American Academy of Pediatrics, Pediatr., 115, 496 (2005).
CrossRef - Pons S.M., Bargallo A.C., Folgoso C.C. and Sabater M.C.L., Eur. J. Clin. Nutr., 54, 878 (2000).
CrossRef - Goedhart A.C. and Bindels J.G., Nutr. Res. Rev., 7, 1 (1994).
CrossRef - Qian J., Chen T., Lu W., Wu S. and ZHU, J., J. Paediatr. Child Health, 46, 115 (2010).
CrossRef - Barness L.A., Dallman P.R., Anderson H., Colipp P.J., Nichols B.L., Walker W.A. and Woodruff C.W., Committee on Nutrition, 65, 4, 854 (2001).
- ANON, 2011. Breastfeeding benefits for mothers. INFACT Canada.
- Naylor A.J. and Wester R.A., Wellstart Int., 3, 1 (2009).
- Institute of Medicine, The National Academy Press, 6, 113 (1991).
- United Nations Children’s Fund, 1992. Breastfeeding counselling. New York: WHO/UNICEF/IBFAN.
- United States Breastfeeding Committee, 2002. Benefits of breastfeeding. United States: USBC.
- American Dietetic Association, J. Am. Diet. Assoc., 109, 1926 (2009).
CrossRef - Ghaderi R. and Makhmalbaf Z., Iran. J. Allergy Asthma Immunol., 4, 129 (2005).
- Dattner A.M., Clin. Dermatol., 28, 1, 34 (2010).
- Statistics Mauritius, 2011. Population and Vital Statistics. Mauritius: CSO.
- Agency for Healthcare and Research Quality, 2007. Breastfeeding and maternal and infant health outcomes in developed countries. Boston: AHRQ.
- Beral V., Bull D., Doll R. and Peto R., The Lancet, 360, 9328, 187 (2002).
- Bernier M.O., Plu-Bureau G., Bossard N., Ayzac L. and Thalabard J.C., Hum. Reprod., 6, 4, 374 (2000).
- Gartner L.M., Black L.S., Eaton A.P., Lawrence A.P., Naylor A.J., Neifert M.E., O’Hare D. and Schanler R.J., Am. Acad. Pediatr., 100, 6, 1035 (1997).
- Davies H.A., Clark J.D.A., Dalton K.J. and Edwards O.M., Brit. Med. J., 298, 1357 (1999).
CrossRef - Danforth K.N., Tworoger S.S., Hecht J.L., Rosner B.A., Colditz G.A. and Hankinson S.E.,.Cancer Causes Control.,18, 5, 517 (2007).
- Rosenblatt K.A. and Thomas D.B., Int. J. Epidemiol., 24, 3, 499 (1995).
- La Leche League International, 2009. Breastfeeding- benefits for mother [online]. Available from: http://www.childfun.com/index.php/parenting/breastfeeding/1092-breastfeeding-benefits-for-the-mother.pdf
- Eglash A., Montgomery A. and Wood J., Disease-a-Month, 54, 6, 343 (2008).
- Health Service Executive, 2008. Contraindications to breastfeeding. Ireland: HSE.
- Giugliani E., J. Pediatr., 80, 5, 147 (2004).
- Ohio State University Medical Center, 2007. Breastfeeding problems. Mount Carmel Health: Ohio University.
- Brent N., Rudy S.J., Redd B., Rudy T.E. and Roth L.A., Arch. Pediatr. Adolesc. Med., 152, 1077 (1998).
CrossRef - Uvingstone V.H., Goutt P.W., Crickmer S.D., Fox K. and Prior J.C., Clin. Endocrinol., 41, 193 (1994).
CrossRef - Renfrew M., Dyson L., Wallace L., D’Souza L., McCormick F. and Spiby H., National Institute for Health and Clinical Excellence, 1, 1 (2005).
- National Academy of Sciences, 2004. Infant formula. US: National academy of sciences.
- World Health Organisation, 2009. Infant and young child feeding. France: WHO.
- Mannheim J.K., Kaneshiro N.K. and Zieve D., 2010. Infant formulas-overview [online]. Available from: http://www.umm.edu/ency/article/002447.htm
- Fisher R.J., Medicine Today, 8, 39 (2007).
- Disanto J. and Disanto K.Y., 2012. Breastfeeding vs. Formula Feeding [online]. Available from: http://kidshealth.org/parent/growth/feeding/breast_bottle_feeding.html#
- Hirsch L., 2008. Breastfeeding vs. Formula feeding [online]. Available from: http://kidshealth.org/parent/growth/feeding/breast_bottle_feeding.html#
- Davidson T., 2004. Infant Nutrition [online]. Available from: http://www.diet.com/g/infant-nutrition
- World Health Organisation, 2000. Complementary feeding. France: WHO.
- Foote K.D. and Marriott L.D., Brit. Med. J., 88, 488 (2003).
- Kuo A.A., Inkelas M., Slusser W.M., Maidenberg M. and Halfon N., Matern. Child Hlth J., 15, 1185 (2011).
CrossRef - United Nations Children’s Fund, 2012. Complementary feeding and complementary foods [online]. Available from: http://www.unicef.org/programme/breastfeeding/food.htm
- World Health Organisation, 2001. Report of the expert consultation on the optimal duration of exclusive breastfeeding. Switzerland: WHO.
- Weiss R.E., 2011. Weaning your baby [online]. Available from: http://pregnancy.about.com/od/breastfeedinginfo/a/weaning.htm
- Child and Youth Health, 2011. Foods for babies (solids) 1- How and when to start. South Australia: CYH.
- Lindberg L., Bohlin G. and Hagekull B., Int. J. Eat. Disorder,10, 4, 395 (1990).
- Berall G., 2009. Feeding difficulties in infants and young children [online]. Available from: http://www.mednet.ca/IMG/pdf/HO10-001_Eng_with_WM.pdf
- Liu Y.H. and Stein M.T., Encyclopedia on early childhood development, 1 (2005).
- Ray S. Personalized Modification of Breast Milk to Help Enhancing Nutrition Profile of Neonates: A Short Communication.Curr Res Nutr Food Sci 2014;2(1). doi : http://dx.doi.org/10.12944/CRNFSJ.2.1.07
CrossRef

This work is licensed under a Creative Commons Attribution 4.0 International License.





